HIV-Prevention Medications Also Protect Against Genital Herpes
July 3, 2014 by Justin Lehmiller
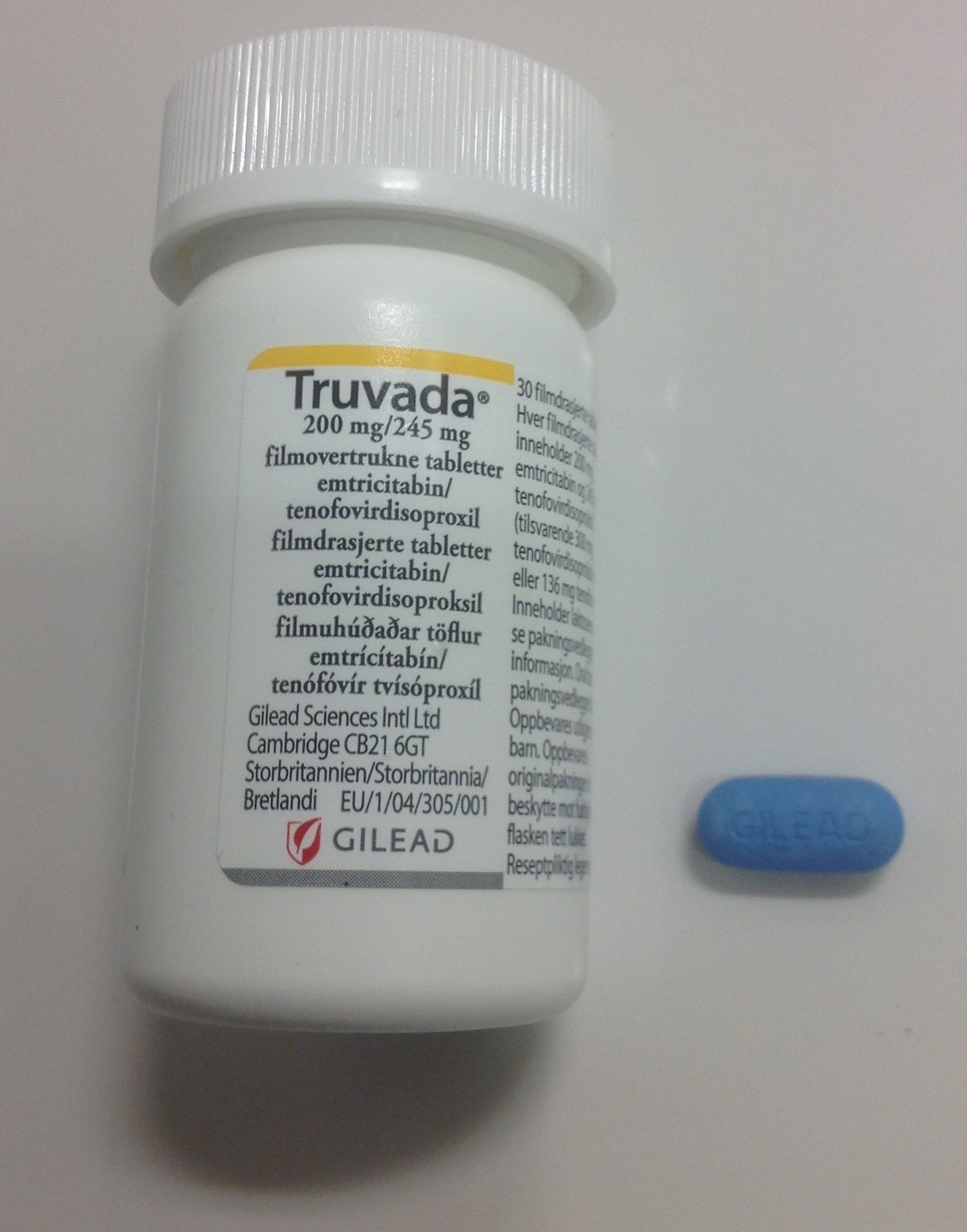
Pre-exposure prophylaxis (or PrEP for short) has been in the news a lot lately. In case you are not familiar, PrEP refers to a new method of HIV prevention. Uninfected individuals simply take a medicine known as Truvada daily (Truvada is a combination of two different drugs, tenofovir and emtricitabine). This is actually the same medication used to treat people who are HIV-positive—and it works for them by dramatically lowering the level of the virus in the body (to be clear, this is not a cure–but it does help extend the life of an HIV-positive person significantly). However, when taken by someone who is uninfected, this drug appears to be effective at preventing the virus from ever taking hold. In fact, some studies have found that among individuals who take this drug consistently, their risk of contracting HIV is reduced by as much as 92%! A new study suggests that PrEP may have the positive side effect of protecting against other sexually transmitted infections as well.
In this study, researchers tracked 1,498 adults in Kenya and Uganda who were taking part in a larger clinical trial for PrEP. Participants were randomly assigned to one of three conditions: Truvada (which, as previously mentioned, is a combination of tenofovir and emtricitabine), tenofovir only, or placebo. In each case, participants took one pill daily.
Participants enrolled in the study between 2008 and 2010 and were followed until July 2011. Participants were tested to see whether they contracted HIV and/or genital herpes over the course of the study.
As you would expect, those who took PrEP had a significantly lower likelihood of contracting HIV [1]. Specifically, for those who took Truvada, they were 75% less likely than the placebo group to contract HIV. Likewise, those who just took tenofovir had a 67% lower risk.
PrEP was also related to a lower risk of contracting genital herpes (specifically, the type 2 variant of the herpes simplex virus, also known as HSV-2), but the drop was not quite as large as it was for HIV [2]. For those who took Truvada, their risk of genital herpes was reduced 36% relative to the placebo group. Those who just took tenofovir had a 24% lower risk.
So why does PrEP also provide some protection against genital herpes? The authors of this study point out that lab research has found that tenofovir appears to inhibit replication of HSV-2 in bodily tissues. In light of such results, it is not all that surprising that PrEP also had an effect on risk of genital herpes in this clinical trial.
On a side note, this study did not look at the risk of contracting oral herpes, known more commonly as “cold sores” or “fever blisters.” Oral herpes is usually caused by the type 1 variant of the herpes simplex virus, or HSV-1, which was not tested here. So we must await future research to see if PrEP protects against both genital and oral herpes.
Overall, these results are encouraging, especially because having herpes increases the risk of HIV transmission and acquisition (during a herpes outbreak, the sores that appear create a direct pathway into the body). A drug that prevents both herpes and HIV is thus a very positive development.
However, don’t expect doctors to start administering PrEP to people who are concerned about herpes only. For one thing, Truvada (like any medication) has side effects. People who are on it also need to have their liver screened regularly for toxicity. However, perhaps the biggest issue is the price tag—in the US, Truvada currently costs about $1,000 per person, per month. That’s simply too much money to spend trying to prevent a non-lethal virus like herpes, especially in light of the fact that the drug only provides modest protection from it. In a world with limited healthcare resources, it is therefore only feasible and affordable to use Truvada primarily for HIV prevention among those persons who are at the highest risk of contracting it.
Lastly, it’s important to remember that Truvada isn’t an excuse to stop using condoms. For one thing, Truvada isn’t 100% effective at preventing HIV. And for another, HIV isn’t the only sexually transmitted infection out there that matters. So, even though Truvada provides protection from HIV and (to some extent) genital herpes, it is not a replacement for safe sex.
Want to learn more about Sex and Psychology? Click here for more from the blog or here to listen to the podcast. Follow Sex and Psychology on Facebook, Twitter (@JustinLehmiller), or Reddit to receive updates. You can also follow Dr. Lehmiller on YouTube and Instagram.
[1] Baeten, J. M., Donnell, D., Ndase, P., Mugo, N. R., Campbell, J. D., Wangisi, J., … & Celum, C. (2012). Antiretroviral prophylaxis for HIV prevention in heterosexual men and women. New England Journal of Medicine, 367(5), 399-410.
[2] Celum, C., Morrow, R. A., Donnell, D., Hong, T., Hendrix, C. W., Thomas, K. K., … & Baeten, J. M. (2014). Daily oral tenofovir and emtricitabine–tenofovir preexposure prophylaxis reduces herpes simplex virus type 2 acquisition among heterosexual HIV-1–uninfected men and women. Annals of Internal Medicine, 161, 11-19.
Image Source: Wikimedia Commons via Fersolieslava
You Might Also Like:

Dr. Justin Lehmiller
Founder & Owner of Sex and PsychologyDr. Justin Lehmiller is a social psychologist and Research Fellow at The Kinsey Institute. He runs the Sex and Psychology blog and podcast and is author of the popular book Tell Me What You Want. Dr. Lehmiller is an award-winning educator, and a prolific researcher who has published more than 50 academic works.
Read full bio >